Cleveland Clinic Pioneers AI in Brain Wave Monitoring
The Cleveland Clinic is advancing the integration of artificial intelligence (AI) in medical diagnostics by teaching AI systems to analyze brain waves and detect seizures in a fraction of the time it takes human specialists. This breakthrough aims to improve outcomes for epilepsy and stroke patients while addressing a national shortage of trained EEG technologists.
From Hours to Seconds: Transforming EEG Analysis
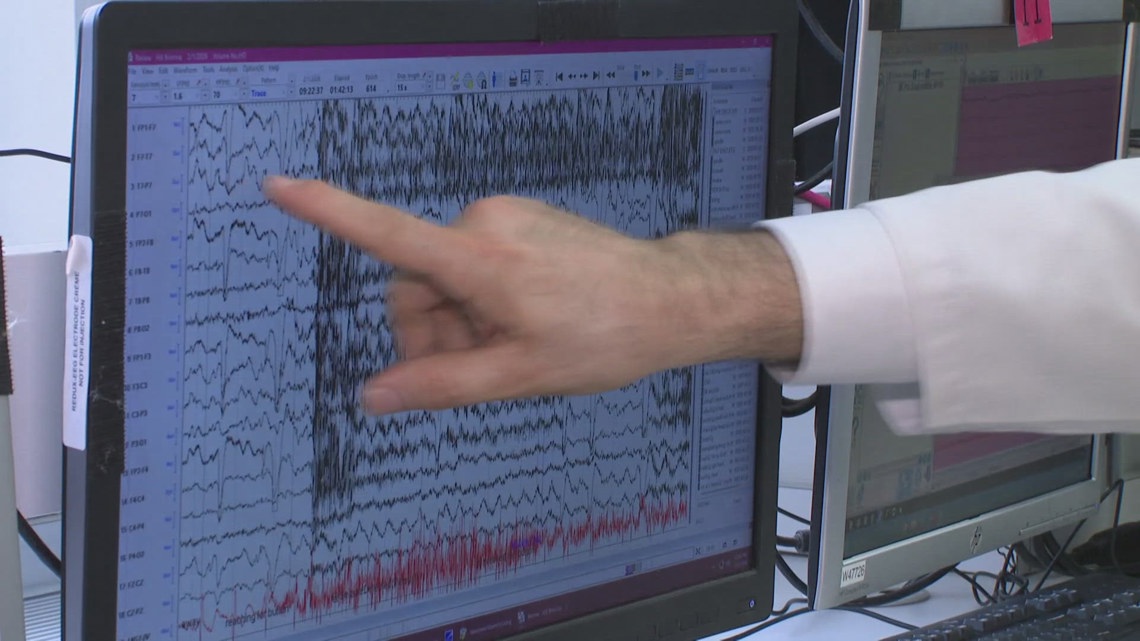
Reading a 24-hour electroencephalogram (EEG) typically takes a specialist about two hours. With AI, that same data can be analyzed in seconds. Dr. Imad Najm, who leads the project, explains that patients in intensive care units (ICUs) require constant monitoring, but staffing limitations make real-time analysis difficult.
“We cannot have enough pairs of eyes to monitor them,” Najm said. “If a patient is having a seizure and we don’t detect it fast enough, their condition can deteriorate rapidly.”
The Evolution of Brain Monitoring
EEG technology has come a long way since Najm started at the Cleveland Clinic in 1992. Back then, EEGs were recorded on paper. Today, digital systems record vast amounts of data, allowing AI to study these readings and identify abnormal patterns. Seizures are characterized by sudden organization in the usually chaotic brain activity, and AI is being trained to recognize this transformation.
Global Centralized Monitoring
In 2010, the Cleveland Clinic established a centralized monitoring unit to oversee patients across its global network—from Ohio and Florida to London and Abu Dhabi. This innovation allows a small team of specialists to monitor over 120 patients simultaneously. However, keeping trained eyes on so many screens at once is impossible, making AI an essential tool.
Teaching AI to Read Brain Waves
Partnering with AI startup Piramidal Inc., the Cleveland Clinic is developing algorithms that replicate human expertise in analyzing EEGs. The AI is trained using a vast dataset of nearly one million hours of recordings, ensuring it can accurately detect seizures and other abnormalities.
“The goal is to make AI as good as we are with our eyes, ears, and brain,” Najm said. “Eventually, it may even see patterns we can’t.”
Improving Outcomes with Early Detection
AI’s ability to detect seizures in real time allows doctors to intervene immediately, potentially shortening ICU stays and improving recovery. When the system identifies a seizure, it alerts the medical team, who can then verify and act on the information.
“Time is of the essence,” Najm noted. “Detecting changes quickly is crucial for patients in critical care.”
Enhancing, Not Replacing, Medical Staff
Rather than replacing human jobs, the AI system enhances the capabilities of existing staff. Trained technologists can focus on high-level tasks while AI handles the initial monitoring. When the AI detects something unusual, it brings the relevant screen to the forefront for immediate review.
“This allows professionals to practice at the level they trained for,” Najm said. “It frees them from the repetitive task of watching multiple screens.”
A Patient’s Perspective
Sarah Beth Himes, an epilepsy patient who has spent significant time wired to EEG monitors, supports the initiative. “Some of my seizures last just a few seconds,” she said. “Monitoring them requires running EEGs for months. AI can help capture those brief events.”
Himes welcomes the technology and looks forward to its future applications. “When they monitor me again, I want them to find out more. It’s worth it.”
Looking Ahead: Seizure Prediction and More
The next frontier is seizure prediction. Researchers hope AI can eventually analyze brainwaves and determine if a seizure is likely to occur minutes in advance. Though this remains a significant challenge, Cleveland Clinic’s extensive data archive may provide the key.
“We’ve tracked patient outcomes for decades,” Najm said. “Now we can group patients by disease and outcome to see what hidden patterns AI might find.”
Scaling Expertise Through AI
Najm envisions condensing the collective knowledge of 28 epilepsy physicians into a single algorithm. “I want to teach AI everything I know,” he said. “That way, we don’t need to spend another decade training someone from scratch.”
This will empower physicians to focus on advancing science and care, using AI to tackle questions previously beyond reach.
Implementation Timeline
The AI system is expected to be ready by the end of summer. It will be tested in parallel with current monitoring practices to ensure accuracy. By early next year, when the Neurological Institute moves to a new facility, the goal is to have the technology fully operational.
“First, we’ll run it experimentally alongside human analysis,” Najm said. “If it performs as expected, we’ll integrate it fully.”
Expanding AI Across Cleveland Clinic
This EEG initiative is part of a broader AI strategy at Cleveland Clinic. Earlier, they implemented AI to detect sepsis, reducing false alarms by 90% and increasing detection rates by 46%. The system now runs in all Cleveland Clinic hospitals across the U.S.
Using real-time data from medical records, the sepsis AI identifies at-risk patients and integrates into physician workflows to prioritize care. Future modules will target additional critical conditions.
This article is inspired by content from Original Source. It has been rephrased for originality. Images are credited to the original source.